Digestive Health Part 11: Too Much Acid

Written by Dr. Claire Arcidiacono, ND acid
For further questions or concerns email me at carcidiacono@invitehealth.com†

Next to constipation and diarrhea, one of the most common concerns that people have is regarding stomach acid. This includes GERD or gastroesophageal re-flux disease. Other common concerns that relate to stomach acid include Peptic ulcers, gastritis, and ironically, too little stomach acid. Since this topic is a complex one to clearly understand, it’ll be broken down into 2 parts.†
So what exactly is GERD or gastroesophageal re-flux disease? GERD is known as acid re-flux or heartburn. The lower esophageal sphincter or “doorway” between the stomach and esophagus doesn’t close properly causing the acid and other stomach contents to leave the stomach and enter the esophagus. Normally the stomach has protections so it’s able to handle the acid without being damaged or causing pain. In contrast, the esophagus doesn’t have these protections and thus when the acid rises up it causes complications and pain.(1)†
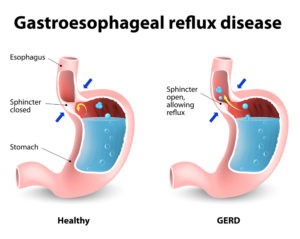
While most people know the symptoms of GERD include heartburn or burning in the chest, it can have quite a few other symptoms or be asymptomatic. In addition to heartburn, there can be a metallic or acid like taste in the mouth. In my practice, this is actually one of the things I always ask people since it’s a classic symptom of GERD even if there is no burning feeling. The acid can cause bad breath and even an increase in saliva. As the acid causes damage, pain with swallowing or even just a chronic sore throat is common. Some people with GERD never have any pain, but do develop symptoms such as a chronic cough, trouble breathing, increase in asthma attacks and even chest pain that can be confused as coming from other things such as the heart. This is typically known as silent GERD since the classic heartburn is absent. While GERD can cause nausea or vomiting, this is less common in adults and is actually seen more in children and infants. (3) Children and infants can get GERD but the symptoms are actually different than in adults. They can include vomiting, spitting up, coughing, wheezing, and food refusal that leads to weight loss. There can also be excessive burping and bad breath. (4)†
Even worse, over time the acid can damage the enamel of teeth as well as the gums. Very often, I see people with dry mouth or burning mouth that turns out to be GERD. (5)†
But what is an ulcer? It’s basically a sore on the inside of you. A Peptic Ulcer is similar to GERD in that the acid is causing the damage either to the stomach (gastric ulcer) or the first part of the intestines (duodenal ulcer). GERD is basically the acid burning a path from the stomach to mouth via the esophageal “highway” where a peptic ulcer has the acid concentrating on 1 spot forming an open sore. (6)†
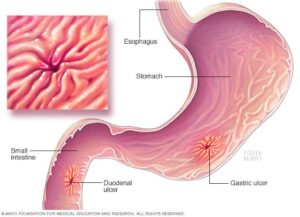
Symptoms of a peptic ulcer that are similar to GERD include an increase in saliva, nausea/vomiting abdominal pain, bloating, vomiting blood, tarry/foul stool and in some cases, heartburn. In a gastric ulcer, you can experience a decrease in appetite vs increase in appetite with a duodenal ulcer. In up to 15% of people there are no symptoms. (8) Gastritis is similar to an ulcer and GERD in that there is inflammation of the stomach lining but unlike an ulcer, it’s not concentrated in one spot.†
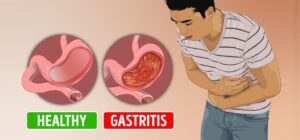
It is very common to have gastritis, an ulcer and/or to suffer from GERD. Symptoms of gastritis can include abdominal pain, nausea/vomiting, heartburn, bloating and gas and even changes in appetite. (10).†
So far everything mentioned is caused by damage due to the stomach acid. But what if there’s not enough acid? In most cases, people have too much acid; not having enough acid can actually contribute to hypochlorhydria or low stomach acid. Signs of hypochlorhydria can include abdominal pain, bloating, gas, diarrhea/constipation and all the symptoms mentioned for GERD/Ulcers and gastritis. Undigested food in the stool is also a sign of hypochlorhydria. Long term, nutritional deficiencies can develop leading to brittle nails, hair loss, paleness, fatigue, numbness, and memory loss. (11)†
Next week we will talk about risk factors for all of these as well as complications. We will also talk about supplements that studies and my own clinical experience have found to be helpful!†
Sources
- “Acid Reflux (GER & GERD) in Adults”. National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). 5 November 2015. Archived from the original on 22 February 2020. Retrieved 21 February 2020.
- https://tulsagastro.com/conditions-symptoms-faq/what-is-gerd/
- Clarrett, Danisa M.; Hachem, Christine (May 2018). “Gastroesophageal Reflux Disease (GERD)”. Missouri Medicine. 115 (3): 214–218. ISSN 0026-6620. PMC 6140167. PMID 30228725.
- Maqbool, Asim; Liacouras, Chris A. (2020). “Normal Digestive Tract Phenomena”. Nelson Textbook of Pediatrics (21st ed.). Philadelphia, PA. ISBN 978-0-323-52950-1.
- Lussi A, Jaeggi T (March 2008). “Erosion–diagnosis and risk factors”. Clinical Oral Investigations. 12 Suppl 1: S5–13. doi:1007/s00784-007-0179-z. PMC 2238777. PMID 18228059.
- Najm WI (September 2011). “Peptic ulcer disease”. Primary Care. 38 (3): 383–94, vii. doi:1016/j.pop.2011.05.001. PMID 21872087.
- https://www.mayoclinic.org/diseases-conditions/peptic-ulcer/symptoms-causes/syc-20354223
- Rao, S. Devaji (2014). Clinical Manual of Surgery. Elsevier Health Sciences. p. 526. ISBN 9788131238714.
- http://aarogyadhamhospital.com/what-is-gastritis-treatment-symptoms-pain-cure/
- “Gastritis”. The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). November 27, 2013. Archived from the original on 6 March 2015. Retrieved 1 March 2015.
- The Gastrointestinal System. In: Kibble JD, eds. The Big Picture Physiology: Medical Course & Step 1 Review, 2e. McGraw Hill; 2020.

