Systemic Lupus Erythematosus (SLE)- Invite Blog

Written by Dr. Claire Arcidiacono, ND
For further questions or concerns email me at carcidiacono@invitehealth.com
Last time we talked about RA, (Rheumatoid Arthritis), which is an autoimmune disease that includes joint pain as well as joint damage. In this same theme we have Lupus. Systemic lupus erythematosus or lupus is a well-known autoimmune disease which involves the body’s very own immune system attacking and damaging healthy cells. Lupus can mimic many different diseases and it is often called the great imitator. Due to this fact it is often misdiagnosed, and thus appropriate treatment is often delayed. † (1)
Lupus very commonly presents with a fever, malaise, fatigue, and both muscle and joint pain. It is interesting to note that while Lupus is much more likely to develop in women it can and does occur in men. The symptoms of lupus are slightly different between the two genders. Typically, women will have a low white blood cell count, increased risk of RA, Raynaud’s syndrome and even a higher rate of psychiatric symptoms. In contrast men tend to experience more seizures, kidney disease, serositis, skin disorders and neuropathy. † (2)
Skin disorders are very common in lupus. In fact, up to 70% of people diagnosed with lupus have symptoms of the disease in their skin. The Malar rash otherwise known as the butterfly rash is a well-known symptom of lupus and occurs in 30-60% of people diagnosed with Lupus. (3) See attached picture. † (4)
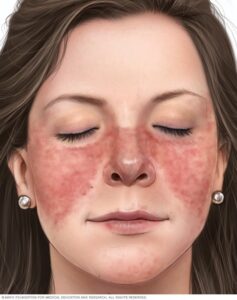
Anemia is very common in lupus and develops in approximately 50% of children who have been diagnosed with lupus. In addition to anemia, it is common to develop low platelet count, low white blood cell count, and different clotting type disorders. As a fascinating aside one of the autoantibodies that are present in lupus is called anti-cardiolipin antibody and it is interesting because it can present a false positive result on a syphilis test. † (5)
Lupus can also present with symptoms that are caused by damage to the internal organs. There can be inflammation in the heart caused by the lupus which can present as pericarditis, myocarditis, endocarditis, and even atherosclerosis occurs more frequently in those with lupus. (6) Similarly, inflammation in the lungs can present with signs of pleurisy, interstitial lung disease, pulmonary hypertension/hemorrhage, and pulmonary embolism. (7) In addition to affecting the heart and lungs it is well documented that lupus can cause inflammation in the kidneys. The inflammation associated with lupus causes symptoms of lupus nephritis in the kidneys. In fact, in lupus immunofluorescence testing shows a very particular granular appearance known as Glomerulonephritis or wine loop nephritis. † (8)
Lupus can also cause neurological symptoms such as signs of neuropsychiatric syndromes. Other neurological symptoms include headaches, seizures, polyneuropathy, cognitive disorders, anxiety, and depression and even in some people psychosis. Other complications include Guillain-Barre syndrome, meningitis, demyelinating syndrome and what are called movement disorders. While lupus has numerous effects on the neurological system, in this article, I have only reviewed the most common. (9) Lupus can also affect the eyes and vision as well. Lupus has been found to affect vision and eye health in up to 1/3 of people that have been diagnosed with lupus. (10) Due to the fact that lupus is an autoimmune disorder there are also effects on fertility. While most people with lupus can and do have healthy children there is an increased risk of miscarriage and the death of the child in utero † (11)
ICYMI:RHEUMATOID ARTHRITIS, INVITE HEALTH BLOG>>READ NOW!
Now you may be saying Dr. Claire this is fascinating but why bring up lupus in a series on joint health. That’s because joint pain is a big part of what lupus is. Now since this is a joint health conversation and not just an arthritis series it is important to talk about lupus since as I said it does affect our joints. More than 90% of those diagnosed with lupus will have joint pain of some degree. While lupus does not usually cause the severe destruction and distortion of the joints seen in RA, there is still joint pain that can vary in its intensity from person to person. It is important to point out that pain is very individualized. Normally a doctor will use a scale from 1 to 10 for patients to rate their pain. What one person would term a 1/10 pain another might feel is an 8/10 on the pain scale. Being more or less sensitive to pain is nothing to be ashamed of. Since we are all different, we all experience pain in a different way. Interestingly there have been studies that suggest a possible link between lupus and RA. At this time more research is needed into this possible correlation. † (12)
Lupus is a complex autoimmune disorder and thus in order to give this topic all the attention it deserves I have decided to split this topic into two parts. The next blog will cover the risk factors for developing lupus, specific tests that can help determine if you have lupus and both conventional as well as complementary approaches to controlling symptoms of lupus. †
REFERENCES
- “Handout on Health: Systemic Lupus Erythematosus”. Www.niams.nih.gov. February 2015. Archived from the original on 17 June 2016. Retrieved 12 June 2016.
- 004). “Gender differences in systemic lupus erythematosus”. Gender Medicine. 1(1): 12–17. Doi: 1016/S1550-8579(04)80006-8. PMID 16115579.
- Harris JP, Weisman MH, eds. (2007). Head and neck manifestations of systemic disease. New York: Informa Healthcare. p. 6. ISBN 9781420017564.
- https://www.mayoclinic.org/diseases-conditions/lupus/symptoms-causes/syc-20365789
- Giannouli S, Voulgarelis M, Ziakas PD, Tzioufas AG (February 2006). “Anaemia in systemic lupus erythematosus: from pathophysiology to clinical assessment”. Annals of the Rheumatic Diseases. 65(2): 144–148. doi:1136/ard.2005.041673. PMC 1798007. PMID 16079164.
- Hahn BH (December 2003). “Systemic lupus erythematosus and accelerated atherosclerosis”. The New England Journal of Medicine. 349 (25): 2379–2380. doi:1056/NEJMp038168. PMID 14681501.
- Henderson LA, Loring SH, Gill RR, Liao KP, Ishizawar R, Kim S, et al. (March 2013). “Shrinking lung syndrome as a manifestation of pleuritis: a new model based on pulmonary physiological studies”. The Journal of Rheumatology. 40 (3): 273–281.
- “General Pathology Images for Immunopathology”. Archived from the original on 2007-05-10. Retrieved 2007-07-24.
- Kasama T, Maeoka A, Oguro N (2016). “Clinical Features of Neuropsychiatric Syndromes in Systemic Lupus Erythematosus and Other Connective Tissue Diseases”. Clinical Medicine Insights. Arthritis and Musculoskeletal Disorders. 9: CMAMD.S37477. doi:4137/CMAMD.S37477. PMC 4718090. PMID 26819561.
- Dammacco R (May 2018). “Systemic lupus erythematosus and ocular involvement: an overview”. Clinical and Experimental Medicine. 18 (2): 135–149. doi:1007/s10238-017-0479-9. PMID 29243035. S2CID 13757311.
- Smyth A, Oliveira GH, Lahr BD, Bailey KR, Norby SM, Garovic VD (November 2010). “A systematic review and meta-analysis of pregnancy outcomes in patients with systemic lupus erythematosus and lupus nephritis”. Clinical Journal of the American Society of Nephrology. 5 (11): 2060–2068. doi:2215/CJN.00240110. PMC 3001786. PMID 20688887.
- Joint and Muscle Pain Archived 2007-11-09 at the Wayback Machine Lupus Foundation of America


