Written by Dr. Claire Arcidiacono, ND
For further questions or concerns email me at carcidiacono@invitehealth.com†

Now that we have gone over joint anatomy and lab work that is important for joint health, it is time to get deeper into our interesting topic. Today we are going to cover osteoarthritis. To start, what exactly is osteoarthritis? Osteoarthritis is a type of joint disease where we see a breakdown of joint cartilage and the underlying bone. (1) While other types of joint disease are caused by a dysfunction of the immune system and can thus affect internal organs in osteoarthritis that is not the case. In other words because osteoarthritis is not an autoimmune condition the damage is limited to the joints.† (2)
Osteoarthritis is what is colloquially called “wear and tear” arthritis. The damage seen in osteoarthritis is caused by anything that leads to mechanical stress on the joint. One of the risk factors for developing osteoarthritis is being overweight since the excess weight puts more stress on the joints than they are designed to handle. Other risk factors include abnormal joint or limb development including those who have limbs of different length, or even previous joint injuries. Those who have very physical jobs may have a higher level of joint stress and have an increased risk of osteoarthritis as a result of that.(3) In individuals with a chronic level of inflammation this inflammation may increase the risk of osteoarthritis.(4) There also appears to be a link between menopause and developing osteoarthritis. Unfortunately as we age the wear and tear of daily living also places stress on the joints and thus advanced age can also be a risk factor for osteoarthritis. (5) Certain health concerns can also increase the risk of osteoarthritis. These can include Alkaptonuria. (6) Other chronic diseases that are risk factors include hemochromatosis, Wilson’s disease, ligament deterioration, obesity, joint infection and cognitional disorders. Ehlers-Danlos syndrome is another risk factor. Yet another risk factor is Marfans syndrome. Any other form of arthritis will increase the risk of osteoarthritis. Diabetes appears to increase the risk of needing a joint replacement surgery due to the osteoarthritis. (7)
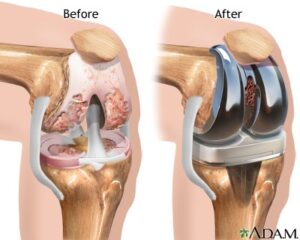
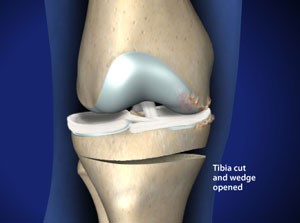
Osteoarthritis is usually diagnosed with a history and clinical exam as well as an x-ray. Getting an x-ray is very important because it can help us understand how severe the illness has progressed. Someone who has the start of osteoarthritis has a very different protocol than someone who has advanced illness. Very often when we speak of arthritis we use the term ‘bone on bone’. What this basically means is that the cartilage has been worn away and the bone is directly rubbing on another bone. Only your doctor can determine if this is the case. From my clinical experience I can tell you I’ve had clients with bone on bone who can walk with what they describe as mild pain. Others with bone on bone can barely walk. Then again I’ve had individuals who are in the early stages of osteoarthritis and they have severe pain. That is why testing is so important.†
One of the first steps in working with osteoarthritis is to lose weight if necessary. The next step is to treat any underlying conditions such as diabetes or any autoimmune conditions you may have. Reducing the stress caused by inflammation can also help reduce the risk of osteoarthritis. (8) A 2015 study showed that water therapy is very helpful for reducing the symptoms of osteoarthritis (9). In addition to any conventional treatments that the doctor may recommend the following have been found in studies to help with osteoarthritis.†
FISH OILS ARE GOOD FOR YOUR JOINTS & KRILL MIGHT BE SUPERIOR- INVITE HEALTH PODCAST, EPISODE 580>>LISTEN NOW!
Dr.Claire’s Recommendations:
Turmeric has been found in studies to help with the pain and inflammation associated with osteoarthritis. It also has been found to help with overall joint health. (10) Please see Invite’s Biocurcumin 5 Loxin, Turmeric with Ginger and Curcumin blend.†
Ginger has been found in studies to reduce the symptoms of osteoarthritis. (11) Please see Invite’s Turmeric with Ginger!†
Collagen has once again been found effective at reducing the symptoms of osteoarthritis in studies! (12)Primary studies indicate that collagen may help to make beneficial changes in the quality of cartilage in osteoarthritis. (13) Please see Invite’s Collagen Hx, Collagex HA, and Cartilage Hx.†
Hyaluronic acid has been found to improve joint lubrication as well as reduce the inflammation found in osteoarthritis. (14) Please see Invite’s Hyaluronic acid with devils claw as well as Invite’s Collagex Ha.†
Glucosamine is very controversial. However while more research is needed it has been found in some studies to help slow the degeneration of the cartilage that occurs during osteoarthritis. (14). Please see Invite’s Glucosamine Chondroitin, Joint Hx and Collagex Ha.†
Omega 3 have been found in newer studies to help reduce the symptoms, for example pain associated with osteoarthritis. (14) Please see Invite’s Fish oil, Krill oil, Biomega and Inflammune.†
Next week we will be talking about Rheumatoid Arthritis!
REFERENCES
1. Arden N, Blanco F, Cooper C, Guermazi A, Hayashi D, Hunter D, Javaid MK, Rannou F, Roemer FW, Reginster JY (2015). Atlas of Osteoarthritis. Springer. p. 21. ISBN 978-1910315163. Archived from the original on 8 September 2017.
“Osteoarthritis”. National Institute of Arthritis and Musculoskeletal and Skin Diseases. April 2015. Archived from the original on 18 May 2015. Retrieved 13 May 2015.
2.Glyn-Jones S, Palmer AJ, Agricola R, Price AJ, Vincent TL, Weinans H, Carr AJ (July 2015). “Osteoarthritis”. Lancet. 386 (9991): 376–387. doi:10.1016/S0140-6736(14)60802-3. PMID 25748615. S2CID 208792655.
3.Berenbaum F (January 2013). “Osteoarthritis as an inflammatory disease (osteoarthritis is not osteoarthrosis!)”. Osteoarthritis and Cartilage. 21 (1): 16–21. doi:10.1016/j.joca.2012.11.012. PMID 23194896.
4.Tanamas SK, Wijethilake P, Wluka AE, Davies-Tuck ML, Urquhart DM, Wang Y, Cicuttini FM (June 2011). “Sex hormones and structural changes in osteoarthritis: a systematic review”. Maturitas. 69 (2): 141–156. doi:10.1016/j.maturitas.2011.03.019. PMID 21481553.
5.Ranganath LR, Jarvis JC, Gallagher JA (May 2013). “Recent advances in management of alkaptonuria (invited review; best practice article)”. J. Clin. Pathol. 66 (5): 367–373. doi:10.1136/jclinpath-2012-200877. PMID 23486607. S2CID 24860734.
https://en.wikipedia.org/wiki/Osteoarthritis#cite_note-23
6.Cibulka MT, White DM, Woehrle J, Harris-Hayes M, Enseki K, Fagerson TL, et al. (April 2009). “Hip pain and mobility deficits–hip osteoarthritis: clinical practice guidelines linked to the international classification of functioning, disability, and health from the orthopaedic section of the American Physical Therapy Association”. The Journal of Orthopaedic and Sports Physical Therapy. 39 (4): A1-25. doi:10.2519/jospt.2009.0301. PMC 3963282. PMID 19352008.
7.Lu M, Su Y, Zhang Y, Zhang Z, Wang W, He Z, et al. (August 2015). “Effectiveness of aquatic exercise for treatment of knee osteoarthritis: Systematic review and meta-analysis”. Zeitschrift für Rheumatologie. 74 (6): 543–552. doi:10.1007/s00393-014-1559-9. PMID 25691109. S2CID 19135129.
8.https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7812094/
9.https://pubmed.ncbi.nlm.nih.gov/11710709/
10.https://pubmed.ncbi.nlm.nih.gov/30368550/
11.https://pubmed.ncbi.nlm.nih.gov/21251991/
12.https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5814393/
13.https://www.mayoclinic.org/drugs-supplements-glucosamine/art-20362874
14.https://www.sciencedaily.com/releases/2011/10/111017111600.htm