Written by Dr. Claire Arcidiacono, ND
For further questions or concerns email me at carcidiacono@invitehealth.com

Last week we started off our discussion of arthritis with osteoarthritis (OA). This week we will be looking at rheumatoid arthritis (RA). When most people think of RA they think of joint pain and while that is true RA is much more than just a joint disease. RA is an autoimmune disorder which involves the immune system attacking the joints. This inflammatory response affects both the cartilage and the underlying bone. However, unlike in OA where other parts of the body are relatively unaffected in RA multiple systems are affected by the disease. In RA for example the skin, eyes, lungs, heart, nerves and even the blood vessels can all be affected. † (1)
The first signs of RA involve the joints. Typically, the affected joints will be swollen, warm and in the morning, they will be very stiff and need to be “warmed up” as people say. Interestingly this is different from the joint pain we see in OA where there is no difference in the morning meaning that there is no morning inflammation or morning joint pain that just needs to be “warmed up”. As the autoimmune disease progresses in its severity the underlying tendons can become affected, and this leads to the structural changes typically seen in RA. I would like to point out that in addition to the structural changes seen in the fingers there can often be similar structural changes in the toes. This is important since it can affect mobility in the long run. (2) Please see the attached pictures. † (3) (4)
Fingers
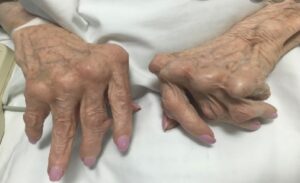
Toes
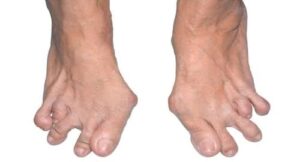
As I said earlier due to the fact that RA is an autoimmune illness other parts of the body are affected and will show signs of the illness. As I discuss each individual aspect of the disease, I will go over how the systems are affected. To start with the very beginning the skin can develop something called a rheumatoid nodule. These typically occur over areas such as the elbow, heels, and the knuckles. † (5) Please see picture (6)
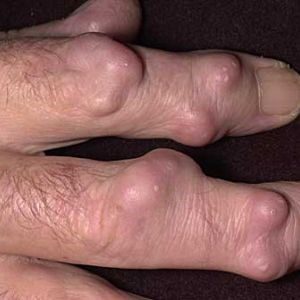
Additionally, vasculitis, which is inflamed blood vessels, can also occur in the skin. Other symptoms of RA that can occur in the skin include but are not limited to the following: Pyoderma gangrenosum, sweets syndrome, Erythema nodosum and even atrophy of the skin of the fingers. † (7)
RA can also affect the lungs and cause signs of respiratory illness. In fact, having symptoms of lung disease when you have RA is so common it even has a name – Rheumatoid lung disease or lung fibrosis. As I said this is a well-known complication of RA. Caplan syndrome is a diagnosis that describes lung nodules that occur when RA is present. † (8)
In addition to symptoms of lung disease individuals with RA often experience comorbidity of the heart and blood vessels. For example, these can include an increased risk of atherosclerosis, MI, and stroke. Other possible complications can include pericarditis, endocarditis, valvulitis and fibrosis. † (9)
Anemia as well as a decrease in white blood cells can also occur. When the inflammation is not well controlled, we can also see an increase in platelet count. † (10)
RA can also affect the kidneys and cause symptoms of kidney disease. It can affect the liver as well and cause symptoms of liver disease. In the long run it can even cause vision changes as it affects our eyes. Over time as the autoimmune aspects of RA starts to affect the nerves, we can start to see signs of neuropathy. † (11)
GENERAL SYMPTOMS
The general symptoms of RA include fatigue, low grade fever, malaise, morning stiffness, and periodontal disease. † (12)
COMMON RISK FACTORS
There are some very common risk factors for RA. For those with RA in their family tree the risk of developing RA increases 3 to 5X that of someone without a family history. In fact is estimated that genetics account for 40-65% of sero-positive RA and 20% of sero-negative RA. (13) Smoking has been found to increase the risk of RA 3X compared to nonsmokers! †(14)
Studies have found that having vitamin D levels that are lower than optimum can increase the risk of developing RA. † (15)
Anything that increases inflammation can also increase the risk of RA. This can include the standard American diet, stress and even other autoimmune disorders. As I mentioned in my article series on digestion having leaky gut is a risk factor for all autoimmune disorders including RA. Studies also show a link between RA and gluten sensitivities. † (16)
As I mentioned previously RA is diagnosed with blood work as well as certain imaging tests. Blood work can also be used to monitor the effectiveness of treatments. In addition to any treatments recommend by your doctor the following may be helpful:
WHAT CAN BE HELPFUL?
1. Lifestyle changes such as stop smoking! †
2. Making dietary changes – A Mediterranean diet has been found to be anti-inflammatory in studies! (17) I would also suggest increasing anti-inflammatory foods – such as leafy greens, broccoli, cauliflower, cabbage, brussels sprouts, kale, berries of all types, cherries, oily fish, avocados, olive oil and nuts. † (18)
3. Working on the inflammation part of RA sometimes requires supplements in addition to diet! †
–> Turmeric has been found to lower inflammation and help with the morning stiffness as well as the inflammation seen in RA. (19) Please see Invite’s Biocurcumin, Turmeric with ginger and Curcumin blend! †
–> Boswellia has been found to reduce inflammatory parameters in studies. (20) Please see Invite’s Biocurcumin!†
–> Ginger has been found to reduce inflammatory factors hs-CRP and IL-1β or in other words it helps to reduce the inflammation seen in RA. (21) Please see Invite’s Turmeric with ginger. †
–> Omega 3’s may have an effect on disease activity especially the swollen and crooked joints. (22) Please see Invite’s Fish oil, Krill oil, and Inflammune.†
–> D3 is important to supplement when you are low. † (23)
4. If the leaky gut is causing the inflammation, it’s important to heal the gut! Please refer to my series on GI health. †
START Dr.Claire’s series on GI Health here–>THE BASICS OF DIGESTIVE HEALTH, PART 1>>READ NOW!
5. We also want to work on protecting the joints! †
–> Collagen has been found to lower joint inflammation and joint pain. (24) While more studies on collagen are important to do at this time current studies show that collagen may help to promote the growth of cartilage damaged by OA or RA. (25) Please see Invite’s Collagen Hx, Collagex HA, Collagen tablets and Cartilage Hx!†
–> Hyaluronic acid has been found in studies to help promote cartilage repair as well as reduce inflammation. (26) Please see Invite’s Hylauronic Acid with Devil’s Claw†
6. Lastly let’s protect some of the other organs affected by RA! †
–> For lung health there are a number of products that can help! NAC has been found to improve respiratory function. (27) Black seed is also amazing for lung health and respiratory function. (28) Please see Invite’s NAC and Black seed with Rosemary†
–> Coq10 is amazing for heart health! Please see all Invite’s Coq10 products! †
–>Resveratrol is amazing for so many different areas. It helps the lungs, heart and is just an amazing antioxidant! (29) Please see Invite’s Resveratrol 100mg Hx and our new Resvertrol Max formula†
–> Bilberry has been found in studies to help with vision and eye heath. (30) For this and other amazing eye nutrients please see our Macula Hx and Macula Advanced Hx†
For further questions or concerns email me at carcidiacono@invitehealth.com
REFERENCES
1. “Handout on Health: Rheumatoid Arthritis”. National Institute of Arthritis and Musculoskeletal and Skin Diseases. August 2014. Archived from the original on June 30, 2015. Retrieved July 2, 2015.
2. Majithia V, Geraci SA (November 2007). “Rheumatoid arthritis: diagnosis and management”. The American Journal of Medicine. 120 (11): 936–939. doi:10.1016/j.amjmed.2007.04.005. PMID 17976416.
3. https://www.orthobullets.com/basic-science/9085/rheumatoid-arthritis
4. https://www.thehealthsite.com/diseases-conditions/how-rheumatoid-arthritis-affects-the-foot-and-ankle-b1016-440550/
5. Turesson C (May 2013). “Extra-articular rheumatoid arthritis”. Current Opinion in Rheumatology. 25 (3): 360–366. doi:10.1097/bor.0b013e32835f693f. PMID 23425964. S2CID 21462453.
6. https://www.pcds.org.uk/clinical-guidance/rheumatoid-nodules
7. Genta MS, Genta RM, Gabay C (October 2006). “Systemic rheumatoid vasculitis: a review”. Seminars in Arthritis and Rheumatism. 36 (2): 88–98. doi:10.1016/j.semarthrit.2006.04.006. PMID 17023257.
8. arthritis-associated interstitial lung disease: the relevance of histopathologic and radiographic pattern”. Chest. 136 (5): 1397–1405. doi:10.1378/chest.09-0444. PMC 2818853. PMID 19892679.
9. 9). “Evaluating cardiovascular risk in rheumatoid arthritis”. Journal of Musculoskeletal Medicine. 26 (8): 481–494. Archived from the original on 2012-07-23.
10. Gibbs JE, Ray DW (February 2013). “The role of the circadian clock in rheumatoid arthritis”. Arthritis Res Ther. 15 (1): 205. doi:10.1186/ar4146. PMC 3672712. PMID 23427807.
11. de Groot K (August 2007). “[Renal manifestations in rheumatic diseases]”. Der Internist. 48 (8): 779–785. doi:10.1007/s00108-007-1887-9. PMID 17571244. S2CID 28781598.
12. “Handout on Health: Rheumatoid Arthritis”. National Institute of Arthritis and Musculoskeletal and Skin Diseases. August 2014. Archived from the original on June 30, 2015. Retrieved July 2, 2015.
13. Smolen JS, Aletaha D, McInnes IB (October 2016). “Rheumatoid arthritis” (PDF). Lancet. 388 (10055): 2023–2038. doi:10.1016/S0140-6736(16)30173-8. PMID 27156434. S2CID 37973054.
14. Sugiyama D, Nishimura K, Tamaki K, Tsuji G, Nakazawa T, Morinobu A, Kumagai S (January 2010). “Impact of smoking as a risk factor for developing rheumatoid arthritis: a meta-analysis of observational studies” (PDF). Annals of the Rheumatic Diseases. 69 (1): 70–81. doi:10.1136/ard.2008.096487. PMID 19174392. S2CID 11303269. Archived from the original (PDF) on 2021-03-01. Retrieved 2018-04-20.(subscription required)
15. https://www.keckmedicine.org/blog/could-more-vitamin-d-help-relieve-your-rheumatoid-arthritis/#:~:text=Studies%20also%20have%20found%20that,in%20the%20hands%20and%20feet.
16. https://pubmed.ncbi.nlm.nih.gov/33677948/
17. https://www.eatingwell.com/article/2061785/anti-inflammatory-mediterranean-diet-plan/#:~:text=In%20fact%2C%20research%20has%20identified,oil)%20in%20the%20diet%20every
18. https://www.healthline.com/nutrition/13-anti-inflammatory-foods
19. https://pubmed.ncbi.nlm.nih.gov/33914984/
20. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6477955/
21. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7137811/
22. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7362115/
23. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3539179/
24. https://www.versusarthritis.org/about-arthritis/complementary-and-alternative-treatments/types-of-complementary-treatments/collagen/#:~:text=Four%20trials%20tested%20collagen%20against,the%20trials%20against%20a%20placebo.
25. https://blog.designsforhealth.com/node/1375
26. https://www.arthritis-health.com/treatment/injections/what-hyaluronic-acid#:~:text=Hyaluronic%20acid%20helps%20in%20the,by%20injury%20or%20tissue%20degeneration.
27. https://www.lifeextension.com/magazine/2020/ss/protect-your-respiratory-system#:~:text=NAC%20(N%2Dacetyl%2DL,%2C%20MD%2C%20in%20May%202022.
28. https://www.webmd.com/vitamins/ai/ingredientmono-901/black-seed#:~:text=Taking%20black%20seed%20oil%20by,low%20lung%20function%20before%20treatment.
29. https://www.webmd.com/diet/health-benefits-resveratrol#:~:text=Resveratrol%20has%20antioxidant%20and%20anti,for%20arthritis%2C%20and%20skin%20inflammation.
30. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7146147/













